Egg binding occurs when an egg gets stuck in the reproductive tract causing the hen difficulty in laying it. The recommended treatment is to support the hen in whatever ways possible to lay the egg: a hot Epsom salt bath to relax the muscles and calcium (crushed Tums in water) to help with the contractions. Inserting lube into the vent can help ease the egg out. If it becomes necessary, you may have to break the egg internally and carefully extract all the contents.
Egg binding usually occurs in young layers or when attempting to lay very large eggs. Other causes include: calcium deficiency, obesity, oviduct infections or the use of supplemental light to force laying year round.
Here’s Sheri’s story treating her young egg bound hen.
Hiwa, Black Copper Marans Hen, 8 months old
She started laying in November and consistently laid abnormal eggs: soft shell, no shell and other issues, but was otherwise healthy.



Day 1-3: Hiwa presented with a number of symptoms: a squishy, extended crop the size of a softball, but no sourness; white urates and watery poop, which suggested an impacted crop.
Day 4: After four days of treating her for sour/impacted crop by massaging her crop, Sheri took her to a 24/7 animal hospital with three main Avian Veterinarians. They found that she actually didn’t have sour crop or any kind of gastro-intestinal obstruction. Her x-rays and ultrasound revealed that Hiwa was egg bound and her crop issues were a side effect of the two large, irregular eggs pressing on her digestive tract.
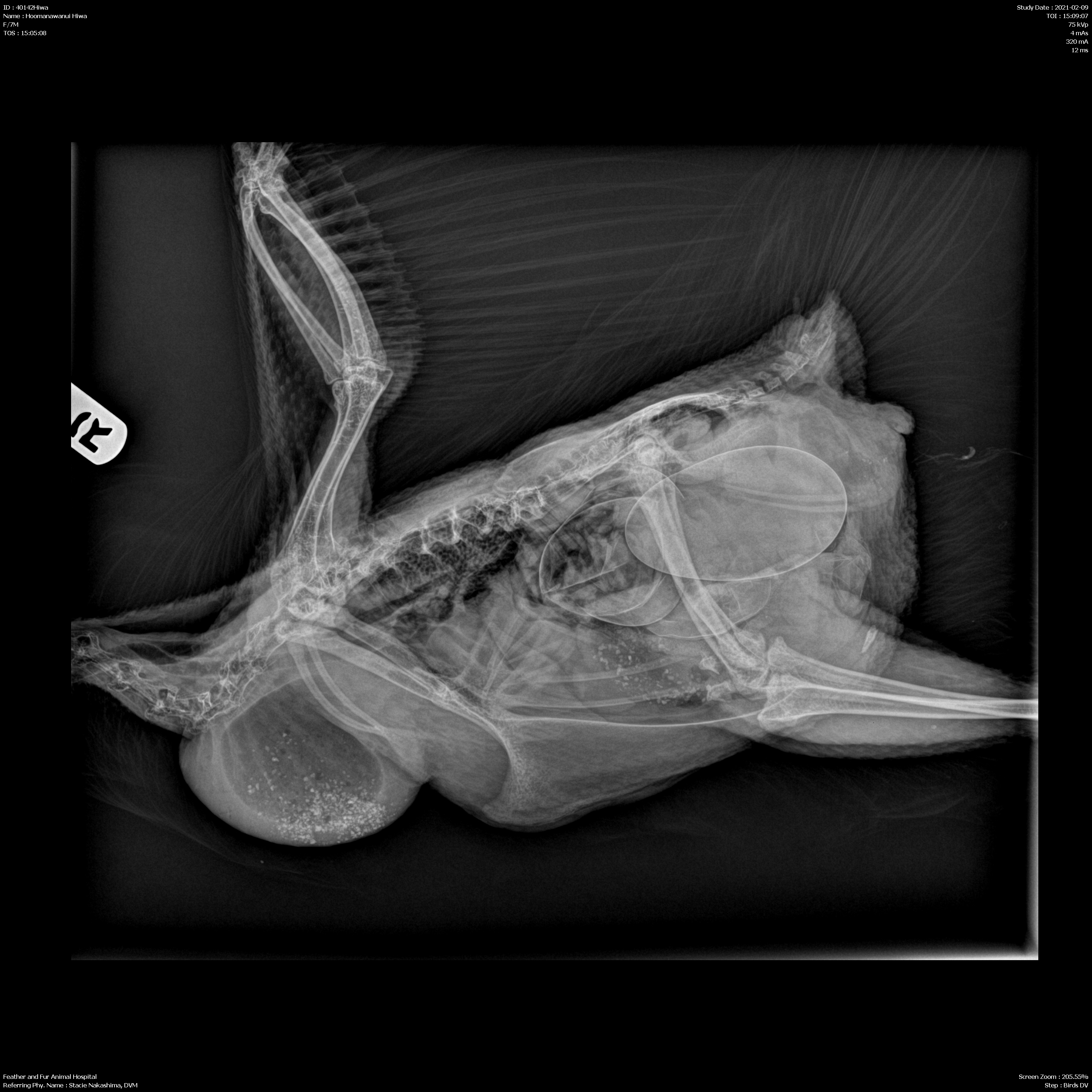

They kept Hiwa overnight and did a digital internal exam and athough they could feel the egg, weren’t sure if it was stuck. The vet also flushed her crop and tube fed her, but could only give her 10cc before she started regurgitating. They recommended she stay several days longer to be tube fed and monitored. She was put on antibiotics (Clavamox) and a pain reliever/anti-inflammatory (Meloxicam). Her normal weight was 3kg; her current weight had dropped to 2.01 kg.
Day 5: There was no movement on the egg, so they were concerned it had adhered to the lining of her oviduct probably because it was soft shelled and due to tissue inflammation. She still was not able to keep down more than 10cc of formula (Emergen-C Intensive Care Omnivore Diet formula). Her weight dropped to 1.9 kg.
Day 6: The vet attempted to manipulate the egg both externally and internally, without success so they used a needle to implode it in order to relieve the pressure and reduce the egg size. The expectation was the egg would pass on its own, but it didn’t. Hiwa’s crop finally emptied and she was able to keep down 20cc of food via tube feeding.
The vets suggested further options: surgery to remove the remnants of the egg because of the risk of egg yolk peritonitis; and to either put Hiwa on hormone therapy or be spayed. The hormone therapy consists of a series of 3 shots, at a cost of $250 each with no guarantee they would work beyond 3-4 months. She might have to be on hormones for her whole life. In contrast, spaying would cost $1500 and hopefully be a permanent solution.
The risk of anesthesia, especially in her weakened state, meant that she had a 50-50 chance of surviving surgery, and then a further 50-50 chance of surviving the first 48 hours post-operation.
Sheri opted to go with the surgery because the vet already had to do surgery to remove the egg debris and, if successful, would be a permanent solution.
As you can imagine birds that have been bred to lay an inordinate amount of eggs are vulnerable to developing a variety of reproductive tract issues: egg binding, internal laying, egg yolk peritonitis and vent prolapse. Most farmers, who raise chickens as livestock, would cull birds that become sick or unproductive. An increasing number of small flock keepers often see their chickens as pets and are willing to spend the time and money on at-home first aid and professional veterinary care. Hens that experience issues with egg laying might be offered a hormone implant that prevents laying or in life-threatening cases the recommendation would be to spay them.
Hormone Implants
Suprelorin (deslorelin acetate) is a hormone implanted under the skin, similar to a microchip, in order to prevent a hen from laying eggs. It is used off-label for chickens and many veterinarians don’t have experience using it in avian species. In hens, the duration of effectiveness can be anywhere from two weeks to two years. It may be administered to a hen pre-spay surgery to stop ovulation and to decrease blood supply to her reproductive organs.
What Is Spaying In Chickens?
Surgery of any kind is a big undertaking both financially and because of the risk of complications, infection or death. Many small animal veterinarians don’t deal with chickens, and those that do may have limited surgical experience.
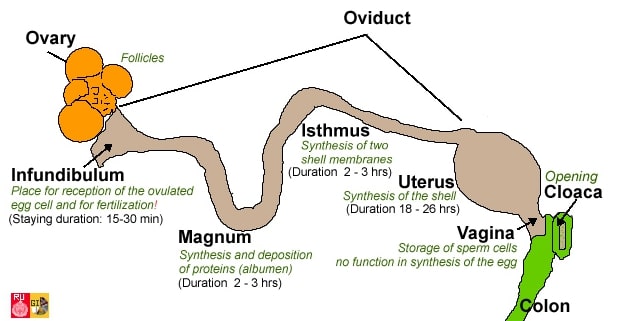
Spaying a hen usually involves the removal of the oviduct rather than the ovaries, which is more risky due to their increased blood supply and close proximity to the aorta. Removal of the oviduct usually prevent the ovary from producing egg follicles, therefore it’s unnecessary to remove them as well.
The risks of this procedure include: overdose of the anesthesia, bleeding out, and complications with the removal of the oviduct due to tumours or adhesions and the necessity to cut through ribs if there is a lot of material to be removed from the oviduct. Post-surgery risks are: infection and the possibility of internal laying if the ovary continues to function. If those eggs aren’t absorbed it can lead to egg yolk peritonitis.
“I had no plans to spend this amount of money, but had already paid $1200 for her hospitalization. The hormone therapy seemed more expensive in the long run and I was genuinely curious what was wrong and how they might fix it. I am a college professor and have dedicated my life to teaching. I thought this would be an opportunity for the vets to do another surgery and get more experience to help someone else and other chickens down the road.” – Sheri
Day 7: The spay surgery was successful. They found a tear at the top of her oviduct and removed the debris of six eggs from her abdominal cavity. Because Hiwa had already been on antibiotics for several days before the procedure she didn’t develop egg yolk peritonitis. She had a lot of inflammation in her reproductive tract, which contributed to the eggs not passing on their own.
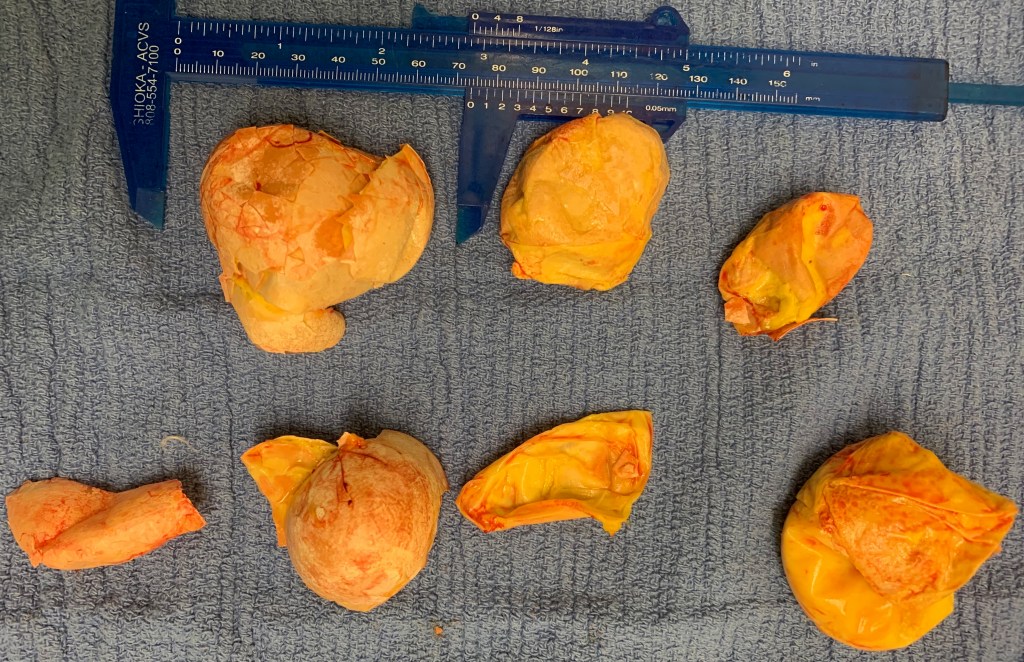
Remnants of Eggs Surgically Removed
Notes From The Veterinarians
I asked Sheri a few questions about the details of Hiwa’s surgery and her vets kindly obliged by answering them in writing:
“When eggs get stuck and we have to implode them, we typically use a needle to insert into the egg and a syringe to remove the contents, then implode the egg with pressure from our fingers. In Hiwa’s case the egg imploded just from touching it because it was not well mineralized because it had ruptured out of the oviduct prior to her admission.
We are unable to remove the ovary because of how close it sits to the major blood vessels, so we removed the entire oviduct from as close as possible to the ovary to as close as possible to the cloaca. Unfortunately we did not take more pictures besides the one posted because we were so focused on the surgery itself and then recovering her. In retrospect it would have been nice to have a few more photos.
We used metal staple-like devices called hemoclips to tie off the ends of the oviduct and remove it. How many I don’t remember, but at least two on each side. Her body was closed in four separate layers with what is called a simple continuous pattern. The four layers were: 1) intra abdominal fat 2) body wall muscle 3) subcutaneous tissue (mostly fat) and 4) skin. Because a simple continuous pattern is one long connected pattern there weren’t individual stitches to count.
Lupron is the name of the injectable hormone suppressor that can help stop birds from laying eggs. However it does not work as well in chickens because of their size and strong egg laying drive. Additionally, in Hiwa’s case those six egg remnants that were outside of the oviduct would have caused a fatal peritonitis if they were not removed, so surgery was definitely her best option.”
Day 8-9: Hiwa was hospitalized post-op and came home with a large supply of oral medications: 10 days of Clavamox (antibiotic), 5 days of Meloxicam and Gabapentin (pain management) and 2 weeks of Terbinafine, an anti-fungal to prevent sour crop which can develop from being on antibiotics for so long. The vet recommended that she eat whatever she wanted in order to gain weight. She wasn’t very hungry while on the antibiotics and healing so her weight dropped to 1.8 kg.
Week 2: It was a struggle to get her to eat anything. She only ate fresh meal worms; defrosted, frozen peas; cooked spaghetti noodles and romaine lettuce, so she continued to lose weight. Sheri learned to tube feed her from a friend and was able to get 40cc into Hiwa twice a day.
At her one week post-op checkup, the vet suggested feeding her 40cc three times a day. Her weight slowly improved, as did her crop issues.
Week 3: She passed her 2 week post-op checkup. Her incisions were all healed and the vet said Hiwa can “go back to being a normal chicken.”
Week 4: 3 weeks post op: Hiwa’s weight was up to 2.1 kg. Because she had been spayed and won’t produce eggs anymore, she probably won’t get back up to 3 kg, but is finally startied to fill out again and was very happy.
Hiwa started to eat her crumble and more of her regular diet and was very active. The only time she appeared sick was when she wasn’t eating much.
Week 5: Hiwa steadily improved – 2.2 kg. She ate her normal diet of Layena crumble (the vet suggested this would help her gain weight), some scratch, mealworms, fresh greens, and discovered a new found love of peas.

Hiwa, 4 weeks after her surgery
Although this was an expensive and stressful undertaking there was a silver lining. Sheri attributes the positives of this experience as all the things she learned from the vets, including how to tube feed. And the best part is now that Hiwa has fully recovered, despite a history of never wanting to be handled, she has become a lap chicken.
A big shout out to Sheri Hoomanawanui for sharing her story and photos; and to the team at Feather and Fur Animal Hospital in Kailua, Oahu, Hawaii: surgeon/medical director Dr. Brian Walsh, Dr. Katie Hancock and Dr. Stacie Nakashima.

Hello. Emma has also had a salpingectomy. Can you please tell me if, in your experience, a hen still has normal hormones and still acts like she wants to lay, is vocal, etc.? Thank you.
LikeLiked by 2 people
Good question. I’ll do a bit of asking around and then post what I find.
LikeLiked by 1 person
Great article. Happy to have all the information I can get about medical care for chickens!
LikeLiked by 1 person
What a blessing to have a veterinarian so capable & committed to a chickens care! Of course, Sheri did most of the work that enabled Hiwa to recover. Great story
LikeLiked by 1 person
All DVMs are trained in mammal medicine. It’s hard to find a vet who actually knows much about birds.
LikeLike
Agreed. I live in a rural area & you have a couple of small animal vets in our county or the ones who deal with horses, goats & cattle. Chickens don’t seem to be high on the list of priorities around here. Not compared to the almighty Longhorn. Then again, I’m not sure how much demand there is for chicken care. This town is still pretty back woods in a lot of ways.
I hope that the number of compassionate chicken keepers continues to grow. As more people get into ducks, guineas, peafowl & turkey, maybe we’ll become enough of a presence for somebody to decide its worth their while to start a practice here. Meanwhile, it’s drive 90 minutes (one way) to get help, but only during business hours. If not, we’re on our own.
LikeLiked by 1 person
I think part of the issue is that avian and mammalian anatomy, physiology and pathology are quite different. Also there are a number of pathogens that affect poultry that don’t affect mammals. It’s kind of like going to your family doctor and expecting them to be familiar with oncology or obstetrics which require specialized training. My mentor is a DVM as well as has a Masters degree in Avian Pathology. She does training with DVMs on basic poultry veterinary care. As more small flock folks see their birds as pets and are willing to take them to a vet more vets will expand their practices to include poultry.
LikeLike